Root canals cause breast cancer – frequently
Breast cancer causes enormous morbidity and mortality around the world, and its traditional treatment, along with the relentless progression of the disease, greatly impacts the quality of life for both patients and their families. This cancer basically targets just women, as only a relatively minimal number of cases occur in men (roughly 1%). [1] Yet, despite its predilection for women, breast cancer is still the most common of malignancies (aside from non-melanoma skin cancers) statistically in the overall population. It continues to be the leading cause of cancer deaths across the planet. [2]
Redox Biology and Toxins
Reduction and oxidation basically refer to the movement of electrons between molecules. When a normal biomolecule with a normal electron content is depleted of one or more electrons, it becomes oxidized. And when that oxidized biomolecule can regain the lost electron(s), it returns to a normal, reduced chemical state. A reduced biomolecule functions normally, while an oxidized biomolecule either partially or completely loses its normal chemical/biological function. More oxidized biomolecules result in the accumulation of largely metabolically inert agents that only occupy space, interfering with normal chemical reactions and no longer directly supporting normal biological function. Examples of biomolecules include sugars, fats, proteins, enzymes, nucleic acids, and structural molecules.
Redox (reduction-oxidation) biology is based on the concept that all biological health is directly due to the degree of reduction versus oxidation in the biomolecules throughout the body. Higher reduction/oxidation ratios indicate good cellular health. This has led to the frequent use of the term “oxidative stress” as the premier biomarker and measuring stick of all disease.
Widely discussed in the medical and scientific literature, increased oxidative stress, or the excess presence of oxidized biomolecules, is always the primary pathophysiology of any disease under consideration. [3,4] It is characterized by a relatively low antioxidant presence and/or an increased pro-oxidant presence. At the cellular level, all diseases or medical conditions have increased oxidative stress in the cells of the affected organs or tissues. The extracellular areas are often involved as well. As pathology cannot exist in the absence of excess oxidation, there are no exceptions to this premise.
All toxins damage by directly or indirectly causing the oxidation of important biomolecules. Oxidation is the chemical process of giving up, or losing, one or more electrons to an electron-robbing toxin (pro-oxidant) that never surrenders that electron back to an oxidized biomolecule once it is acquired. Unless an agent results in the oxidation of biomolecules in the body along with the permanent retention of the electrons it has taken, it is not toxic, and it cannot be toxic. Clinical toxicity and any symptoms of toxicity cannot exist in the absence of excess oxidized biomolecules.
As excess oxidation is the basis of all disease, it logically follows that all cancers, either in the breast or elsewhere, result from excessively and chronically elevated oxidative stress at the affected tissue site. This elevated oxidative stress is always secondary to electron-depleted toxins, also known as pro-oxidants, poisons, free radicals, reactive oxygen species, or oxidizing agents.
This leads to the following two questions:
- What is the source of the toxins in breast cancer, and
- What is causing them to excessively accumulate?
Breast Cancer Pathophysiology
All chronic degenerative diseases, including cancer, only arise when an area of affected tissue becomes substantially inflamed and remains that way. Phrased differently, the areas in the body that have exceptionally increased and chronic oxidative stress are the areas where malignant transformation eventually takes place. Lesser degrees of increased oxidative stress, depending on their location, underlie the development and maintenance of all non-malignant diseases as well. But the highest chronic elevations of oxidative stress, both intracellularly and extracellularly, are the reasons for the initiation and evolution of cancerous growth. No cancer has ever developed in an area that was not already inflamed. While a cancer can metastatically seed abnormal cells in a previously normal tissue site, the primary cancer focus will never be initiated in normal, uninflamed tissue.
A prolonged and sizeable presence of toxins always precedes the development of cancer in the affected areas of the breast. These toxins are produced by slow-growing pathogens (colonizations), and the pathogens themselves will often be found at the cancer site as well. But toxins (highly pro-oxidant molecules) must always be present in order to provoke and sustain a state of chronic inflammation and excess oxidation.
The amount of time that such a toxin/pathogen accumulation needs to be present before a cancer develops is highly variable. Some women with exceptionally strong immune systems, high antioxidant intake, and a relatively lesser degree of toxin/pathogen presence may never demonstrate malignant transformation. Of note, benign breast lumps and other forms of breast pathology result from lesser degrees of toxin exposure.
No pathology of any kind can develop when a tissue has intracellular and extracellular levels of oxidation that are physiological in degree (from normal metabolism). Only increased levels of oxidation can result in pathology. And only extremely increased levels of oxidation result in the appearance of cancer.
In addition to a blood circulation, the body has a lymphatic circulation as well. This circulation moves lymph, the plasma-like extracellular fluid bathing the cells throughout the body, into the venous blood circulation. Under normal circumstances, this lymph flow is one-way only in the direction needed to reach the blood. [5] The primary role of the lymphatic circulation is to provide an outlet for cellular waste products, excess water, and toxins, as well as to support an immune defense against pathogens. [6] It also periodically condenses into focal bodies known as the lymph nodes.
These lymph nodes, of which there are about 500 to 600 in the body, work to concentrate B- and T-lymphocytes needed to combat the infectious agents that are encountered, such that the lymph itself is rendered sterile by the time it leaves the lymph nodes and reaches the blood. [7,8] When draining a large enough source of infection, such lymph nodes will readily enlarge and become sore where they can be felt (palpated), such as in the neck, armpits, or groin areas. Once the processed lymph finally reaches the blood circulation, multiple ways of metabolizing and excreting the remaining non-infective extracellular debris are then available.
The breasts have an extensive lymphatic circulation, and much of its lymph comes from drainage of the head and neck. A portion of the breast lymph subsequently flows into a large collecting vessel (thoracic duct), which then empties into the venous circulation. The rest of it first flows into the extensive lymphatic network in the armpits before eventually reaching the thoracic duct and the blood.
The lymphatic vessels have a limited ability to contract and promote a one-way flow of lymph. [9] However, this lymphatic movement can be slowed, stopped, or even reversed in direction by the presence of sufficient inflammation and structural damage in the tissue being drained. When there is sufficient impairment of normal lymphatic flow, tissue swelling (lymphedema) can result.
In the breast, this impairment of lymphatic drainage can result from either the chronic inflammation in the cancerous tissue, or much more commonly, following the surgical removal of cancer-laden axillary lymph nodes draining the breast. [10,11] The fewer draining lymphatic pathways available, the more likely lymph flow will slow enough to accumulate. Together, both situations result in about 20% of women with breast cancer eventually developing arm swelling due to the back-up of lymph. [12,13]
As with tissues elsewhere in the body, the lymphatic system also drains the superficial gum tissue, the deep gum tissue (periodontium), the teeth, and the tonsils. This drainage largely follows gravity and is filtered in the lymphatic vasculature in the floor of the mouth and then the neck. From there much of the drainage proceeds further down into the rich network of lymphatic vessels in the chest and the breasts, with most of the breast lymph then draining directly into the armpits. [14-16] Deep periodontal infection (periodontitis) has been “linked” to many different cancers, including the breast. Of significant note,
Maintenance of periodontal health has been found to be effective in the primary prevention of breast cancer. This indicates that periodontal infection has a cause-and-effect relationship to breast cancer, not just a link, association, or correlation. [17]
Left unresolved, periodontitis seeds pathogens and their associated toxins throughout the body. To assert that disease occurring after such typical oral pathogens start growing in different tissues is some ill-defined “association” and not a straightforward cause-and-effect relationship defies simple logic. Aside from breast disease and breast cancer, chronically infected gums have been significantly linked to nearly all diseases and conditions. Some studies also document improvement of the “linked” disease with effective periodontitis treatment, as well as a worsening of the disease as periodontitis progresses. This further indicates that periodontitis has a cause-and-effect with most chronic diseases. These diseases and conditions include the following:
- Cardiovascular disease and all-cause mortality, including atherosclerosis, myocardial infarction, heart failure, abnormal lipid and cholesterol metabolism (metabolic syndrome), diabetes, and arterial calcification [18-32]
- Neurological disease, including migraine, seizure, depression, bipolar disorder, dementia, Alzheimer’s disease, Parkinson’s disease, brain abscess and multiple sclerosis [33-53]
- Chronic pulmonary disease, pneumonia, asthma, allergic rhinitis [54-60]
- Vascular disease [61,62]
- Obesity [63,64]
- Inflammatory bowel disease [65-67]
- Inflammatory bone diseases, including arthritis and osteoporosis [68-73]
- Kidney disease [74-76]
- Cancers (pancreatic, lung, liver, colorectal, esophageal, oral cavity and throat, head and neck, stomach, prostate, blood, skin, and cancer in general) [77-92]
- Female infertility and adverse pregnancy and neonatal/birth outcomes [93-95]
- Thyroid disease [96]
- Anemia [97,98]
- Eye disorders [99,100]
- Psoriasis [101-104]
- Ear disorders (hearing loss, vertigo) [105-107]
- Polycystic ovary syndrome [108]
- Autoimmune disease [109-111]
- Erectile dysfunction [112]
- Increased body-wide inflammation (elevated C-reactive protein levels) [113-115]
- Depressed vitamin levels (C and D) and antioxidants [116-122]
The data above on chronic disease and periodontal infection is vital to understanding the impact of root canals and other infected teeth on the general health. Because the pathogens found in infected teeth only come from deep gum infections (except when large cavities allow the pulp to become infected from above), the infections found around the root tips of affected teeth have the same infectious profile as is found in periodontitis. However, the infected teeth, which include all root canal-treated teeth, are even more disease-causing than the infected gums, since they also have the additional following characteristics:
- The infected teeth have a much greater amount of infectious material, often manifest as root tip (apical) abscesses on X-ray.
- The infectious content in and around the root tips of the infected teeth drains directly into the venous circulation.
- The infectious content in and around the root tips of the infected teeth are also released into the extracellular fluid and drained directly into the lymphatic system of the teeth and jawbone.
- The act of chewing on the infected teeth greatly magnifies the expression of pathogens and toxins into the blood and lymph, as extraordinary pressures are generated between opposing teeth. Since pathogen release into the lymph occurs in addition to their release into the venous blood, the delivery of these oral pathogens and toxins to the entire body is more effective and efficient with chewing on infected teeth than if the pathogens and toxins were just directly injected into a vein with a syringe.
The release of highly pathogenic bacteria into the blood during a root canal procedure has been clearly documented. Of note, their release occurs in the absence of any chewing pressure that would further promote pathogen release. [123,124]
Traditional dentists and endodontists (root canal specialists) somehow deny and/or blind themselves to the massive documentation that all root canals are infected. Instead, they collectively maintain that a successful root canal procedure leaves the tooth infection-free just because a root tip abscess was reduced in size and the pain associated with the acute abscess was relieved.
Nevertheless, all the research on the impact of periodontitis and abscessed teeth on all chronic disease applies to all root canals as well, regardless of how well they were performed technically. Although less extensively studied than the relation of just periodontitis with chronic diseases, a great deal of research has also established a link between chronically abscessed teeth (CAP-chronic apical periodontitis) and many different diseases. CAP simply means an extension of and a more advanced form of deep gum inflammation and infection (periodontitis), with root tip abscesses seen on imaging. Significant research studies have documented this abscessed tooth-chronic disease link, which includes all root canals that have resulted in the reduction of root tip abscesses on imaging studies. These studies directly mirror the many studies on early periodontitis and chronic diseases cited above and include the following:
- Cardiovascular disease [125-130]
- Neurological disease [131-137]
- Eye infection [138]
- Inflammatory bowel disease (including Crohn’s disease and chronic ulcerative colitis) [139-142]
- Diabetes [143]
- Liver disease [144,145]
- Kidney disease [146,147]
- Inflammatory bone diseases [148-152]
- Autoimmune disease [153,154]
- Adverse pregnancy outcomes [155,156]
- Increased body-wide inflammation (elevated C-reactive protein levels) [157-161]
- Reservoir for a wide variety of pathogens (bacteria, fungi, and viruses, including Epstein-Barr and herpes) [162-166]
- Increased morbidity and mortality in COVID-19 patients [167]
- Decreased physical fitness/capacity [168]
- Body-wide disease in general [169]
While other factors may be involved, it appears likely that men have virtually no breast cancer because the amount of breast tissue is so much smaller than in women, and there is much less toxic and infected lymph from oral cavity infections getting continually filtered in that tissue. And even though there is a large difference in the average amount of breast tissue between men and women, the lymphatic drainage patterns are largely the same. [170] Also, larger and denser breasts, along with overly constrictive bras and clothing, can all impede the rate at which lymph can be conducted through the breasts. Anything that slows lymphatic flow, especially if it has a significant toxin/pathogen content, will be a factor in determining whether significant inflammation is allowed to take hold in an area of the breast draining the lymph from the oral cavity. Consistent with this concept, studies have shown that very large-breasted women who undergo breast reduction surgery lower their chances of breast cancer. [171] Furthermore, it has been shown that women with larger breasts fare worse with breast cancer than women with smaller breasts. [172]
Root Canal-Treated Teeth
The root canal procedure is one of the most common dental procedures. A meta-analysis revealed that more than half of the subjects in the populations studied had at least one root canal. [173] A very large review and meta-analysis also found that at least half of the population has at least one abscessed tooth. [174] When combined with the prevalence of abscessed teeth that have not received a root canal treatment, the prevalence of infected teeth runs between 55% and 70% of the subjects in the studies. [175-180] Depending on the information source, between 25 and 45 million root canal procedures are performed in the United States every year. Even the low side of the estimate means that a significant majority of adults are always chewing on one or more infected teeth.
Another study found that over 60% of people in Europe had abscessed teeth, with the prevalence steadily increasing with age. [181] Furthermore, fully 25% of teeth that have had procedures other than root canal treatments end up chronically abscessed as well. [182]
Root canal-treated teeth are generally performed when a patient presents with a painful, acutely-abscessed tooth. The “successful” root canal procedure results in a tooth that no longer hurts, resulting in a happy patient and satisfied dentist, at least for the moment. However, the infection remains as long as the tooth remains unextracted, or when the socket infection remains is not completely cleaned out after extraction.
There is an enormous variety and a large total number of different pathogens and other microbes found in and around the root tips of root canal-treated teeth. Fungi, viruses, protozoa and over 460 different types of bacteria have been identified in these infections. [183] No two root canals have the same assortment of indwelling pathogens, and this is why no two root canals inflict the same degree of infectious/toxic damage to the body. Nevertheless, even the “least toxic” root canals can wreak havoc throughout the body.
The physiological core of the tooth, known as the pulp, contains the nerves, blood vessels, and connective tissue matrix that keep the tooth alive and viable. Once this pulp has become infected, there is no way to eradicate the infection and restore the pulp to its normal, health-supporting state. Instead, the removal of the pulp by the root canal procedure permanently prevents immune system access to the pathogens in the tooth, especially in the miles of dentinal tubules extending away from the pulp throughout the tooth structure.
Without immune support, no infection can be resolved. Furthermore, even without the root canal procedure, the infected pulp quickly destroys the pulp structure itself, just leaving a collection of pus and dead (necrotic) cells that can never be returned to normal. Even though pain can still be felt in the root tips embedded in the jawbone, the upper part of the tooth and the pulp is simply a non-vital shell.
In order to stop the immediate infection-causing pain and remove much of the bulk (but never all) of the infection, the root canal procedure drills and routs out as much of the pulp as can be reached, after which it is filled in with an agent to maintain the overall tooth structure. The ends of the pulp space extend to the tooth root tips embedded in the jawbone, and the pulp infection and its necrotic debris effectively “collects” there. This results in well-defined abscesses surrounding the root tips.
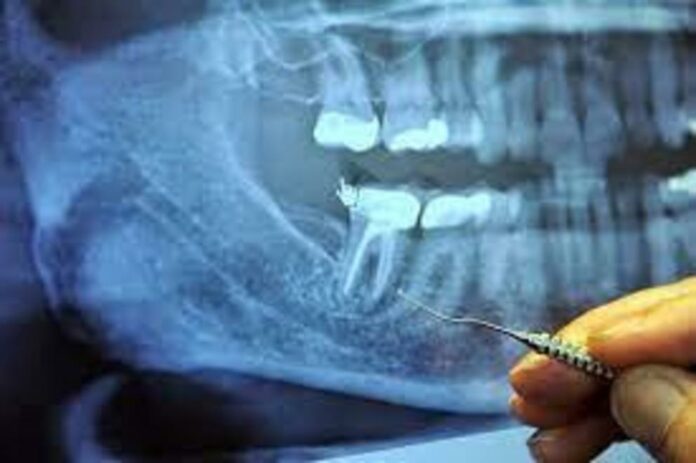
Chronically infected teeth will usually be found to have clearly visible evidence of this pathology at the root tips. On X-ray or on computed tomography studies variably-sized abscesses will nearly always be seen, appearing as dark areas, or radiolucencies, surrounding the root tips. Rarely, the infected tooth might not contain enough infected debris to be visible in an imaging study, but the lack of an identifiable abscess does not mean the infection is still not there.
When a root canal procedure has been performed with optimal expertise, much of the associated root tip abscess will be removed (debulked), and follow-up imaging will no longer easily detect it. However, this does not mean the infection is gone, only that it has been effectively drained. Pathogens and their toxins are still readily expressed into the blood and lymph, especially during chewing.
Dr. Boyd Haley conclusively proved that all root canals produce and collect toxins. He devised a test using a process called nucleotide photo affinity labeling to measure the impact of the pathogen-generated toxins in extracted root canal-treated teeth on five key human enzymes. After studying over 5,000 consecutive extracted root canal-treated teeth sent to him from around the country, the results were stunning. ALL tested teeth had significant toxin content. Differences in the degree of toxicity among the teeth were seen, but none were toxin-free. Such variability in toxicity is to be expected, as no two root canals have the same pathogen population. [184] Furthermore, normal teeth extracted for orthodontic purposes never demonstrated any toxicity, even to a minor degree, ruling out “mouth contamination” as a potential reason for the results.
Of note, Dr. Haley found similar toxin profiles in the specimens sent to him from cavitation surgery. Cavitations occur when chronic infection remains in the healed-over sockets of extracted teeth. [185] Cavitations have a comparable connection to chronic diseases, including breast cancer, although it is much less extensively studied than the relation between abscessed teeth and chronic disease. [186-189]
In addition to the clear visual appearance of chronic infection at the time of extraction, frequently accompanied by putrid odors, ALL root canal teeth extraction sites have pathogens that can be cultured, and microscopic examinations of biopsy specimens always reveal inflamed and necrotic bone and tissue cells resulting from the chronic infection.
For the rest of this article please go to source link below.
For full references please use source link below.